Complex living donor cases possible at Hume-Lee Transplant Center
The Crisses exemplify the difficult cases Hume-Lee will take on.
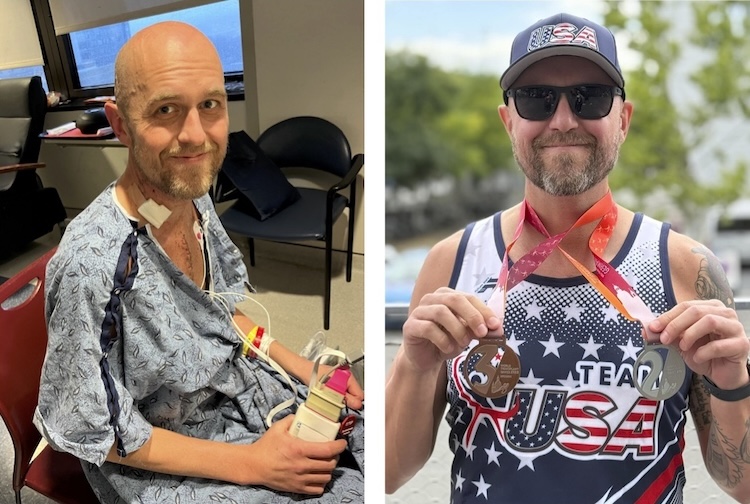
April 07, 2021 Dionne Wynn-Criss and her husband, Al Criss (Photo courtesy of the Crisses)
Dionne Wynn-Criss and her husband, Al Criss (Photo courtesy of the Crisses)
By Jeff Kelley
The VCU Health Hume-Lee Transplant Center is known for its ability to handle the most complex transplant cases. Patients who had been turned down at other centers have been successfully transplanted at Hume-Lee and are thriving.
This includes living donors, who can donate a kidney or part of their liver to someone in need. These individuals undergo a number of tests to ensure a safe and successful donation. But while they may be healthy and a match, their vascular anatomy can be complicated. For example, a patient may have multiple renal arteries and veins or unusually small renal arteries — circumstances that may be too complex for surgeons at other transplant centers.
But not at Hume-Lee. The center specializes in handling complex vascular renal anatomy to make more living donor kidney transplants possible.
“At VCU, we excel at the highly complicated renal anatomy transplants,” said Chandra Bhati M.D., surgical director of living donor kidney transplantation at Hume-Lee.
Alteric “Al” Criss and his wife, Dionne Wynn-Criss, from North Carolina know this firsthand.
From Durham to Richmond
It was early 2020, and Al was suffering from kidney failure. Dionne was by his side.
The couple from Durham, N.C., had a new life-changing routine, which included Al's daily peritoneal dialysis. The time-consuming treatment serves as one of a limited number of options for those suffering kidney failure. The dialysis performs what the kidneys cannot.
Al's illness came as the result of a genetic condition called focal segmental glomerulosclerosis, or FSGS. In this condition, scar tissue develops within the parts of the kidneys that filter waste from the blood (glomeruli).
“I could see dialysis was making him depressed,” Dionne recalled. It held him back from enjoying time with family, especially his young daughter.
On disability as the pandemic raged, Al worried his insurance would run out if the North Carolina medical center where he was being treated kept him waiting for a kidney.
After a family member recommended VCU Health, Al told his doctors he couldn't wait any longer. The couple contacted Hume-Lee.
Pandemic posed obstacles, but Hume-Lee never quit
While it never stopped organ transplants at VCU, the pandemic meant Al couldn’t be seen in person until last May. When the couple finally did make it to the transplant center, a nurse suggested Dionne take a blood test to see if she could be a living donor. Dionne figured she could be, as her blood type was O-negative — the universal donor.
Al recalls the words of Hume-Lee living donor coordinator Maureen Bell: “She says ‘Oh my gosh, sir. If this is true, you just hit the jackpot.’ And I said, ‘Well let me get rich.’”
Living donation has a number of advantages, such as transplanting patients faster. The average wait time for a deceased kidney donor is four to five years. During this time, the patient gets sicker, which makes recovery take longer. In addition, the health and age of most living donors help support strong patient outcomes.
Al and Dionne went back to North Carolina, and a few days later Dionne got the news. She was a match. Al, who was shopping at the time, started crying in the middle of the store.
Surgery goes well
Al received his wife’s kidney on August 4. But not before the surgical team at Hume-Lee deftly navigated Dionne’s unique kidney anatomy. Dionne had two arteries on each kidney as opposed to the single artery most people have. The extra artery is known as an “accessory” artery. In addition, the lower artery on her left kidney was smaller than what most surgeons would prefer.
Many transplant centers will decline the donor if there’s a small accessory artery, noted Bhati, who was Dionne’s living donor surgeon. But the Hume-Lee transplant team was well prepared to handle the case.
“Before the surgery takes place, we knew that we could safely and effectively manage this complex anatomy,” Bhati said.
Dionne’s left kidney was removed and a procedure performed to connect and combine the two arteries on her left kidney. The donor kidney was then successfully transplanted into Al.
Removing Dionne’s kidney was performed using the da Vinci System robot, which gave Bhati far greater freedom of movement, bolstering his steady hands. Bhati was the first on the East Coast to use the da Vinci System for minimally invasive kidney transplants in 2016. Hume-Lee has been a transplant center leader in using this technology.
In addition to minimal scarring and less trauma to the abdominal muscles, the robot also allowed Bhati, chief of Hume-Lee's minimally invasive section of transplant surgery, to dissect a much longer kidney artery. A longer artery is preferred when transplanting kidneys.
Back to a full life
Dionne was discharged after just a day and a half, thanks largely to the fact that robotic surgery leads to less trauma in the body. Al was in the hospital about a week.
Since surgery, Al no longer requires dialysis, and both he and his wife are enjoying active lifestyles. Six months after surgery, Al's creatinine level — a measure of waste in the kidneys — was 1.4, just above the normal but continuing to improve.
“Al is doing very well. His kidney functions are normal, and he's back to his normal life,” Bhati said.
Al and Dionne are glad they reached out to Hume-Lee.
“The experience with the team at VCU was so natural and effortless. They were just like natural family members,” Al said. “The love that they showed and continue to show us every visit and every phone call is totally amazing. We consider them all a part of our family.”
Hume-Lee is committed to safely, effectively and quickly transplanting kidney patients whose health and quality of life continuously decline while on dialysis.
“I encourage every patient who is on dialysis to have a living donor,” Bhati says.
Listen to this podcast featuring living donor Dionne Wynn-Criss on being a living donor. Also featured is Dr. Marcelle Davis, VCU Health director of diversity, equity and inclusion.
Find out more about living-donor transplantation at VCU Health Hume-Lee Transplant Center.