What’s the latest on Alzheimer’s disease? VCU Health expert shares insights
New clinic director highlights the progress in research and treatment of cognitive disorders.
March 31, 2026 About 342,000 people are listed as primary caregivers to Virginians over age 65 living with Alzheimer’s disease. (Getty Images)
About 342,000 people are listed as primary caregivers to Virginians over age 65 living with Alzheimer’s disease. (Getty Images)
By Leigh Farmer
The statistics are staggering – 342,000 people are listed as primary caregivers to the 11.7% of Virginians over age 65 living with Alzheimer’s disease. And the care that these loved ones provide within the commonwealth? It’s estimated to be worth $12.5 billion, according to the Alzheimer’s Association.
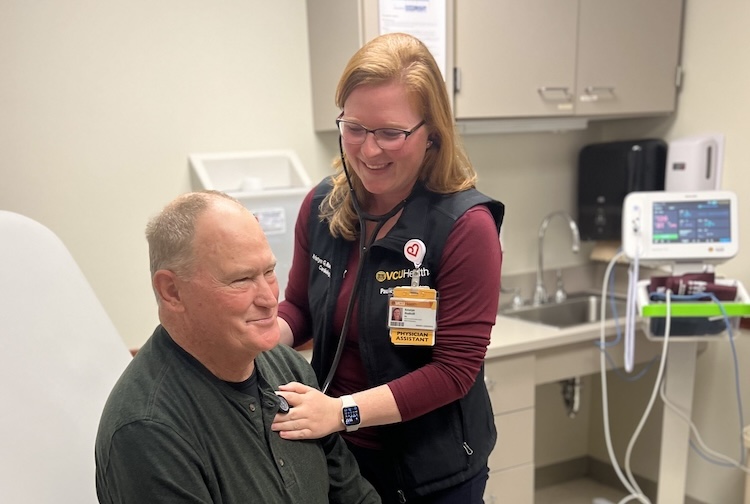
“The need for dementia care in Central Virginia is immense,” said James “Trey” Bateman, M.D., MPH, director of the VCU Health Alzheimer’s disease and cognitive disorders clinic. “There’s an excellent opportunity to grow a program that excels at clinical care, research and education.”
Families need help coping with the diagnosis and care of those they love, and VCU Health strives to be at the forefront of research and treatment.
Internationally, more than 130 new dementia drugs are in the trial phase, with more on the horizon. Several already in the marketplace are proving that progression of the disease can be slowed if caught early and treated with the correct medication. Researchers are also learning how to tailor drugs to an individual patient’s brain chemistry.
While new to VCU Health, Bateman is already hard at work, developing a multidisciplinary clinic of professionals to treat the whole patient once they are diagnosed with Alzheimer’s or a cognitive disorder. His team includes neuropsychologists, nurses, social workers, speech and occupational therapists, mental health professionals and geriatricians – all working together to provide patients with the latest in care.
VCU Health News caught up with Bateman for insight into the latest treatments for these diseases, the evolution of clinical research into Alzheimer’s and advice for patients and families who must navigate a devastating diagnosis.
What inspired your focus on Alzheimer’s disease and other types of dementia care?
I became very interested in how the brain works in college. The idea that understanding the brain could help us understand behavior was really fascinating to me. When I decided that I wanted to go to medical school, neurology was a natural interest for me. During my training at the University of North Carolina, I met Dr. Dan Kaufer, a behavioral neurologist and the school’s founding director of its memory disorders clinic. He specialized in dementia and became my mentor. After meeting him, nothing really made me waver from the desire to be a behavioral neurologist.
What are the latest tools and technologies used to diagnose Alzheimer’s disease today?
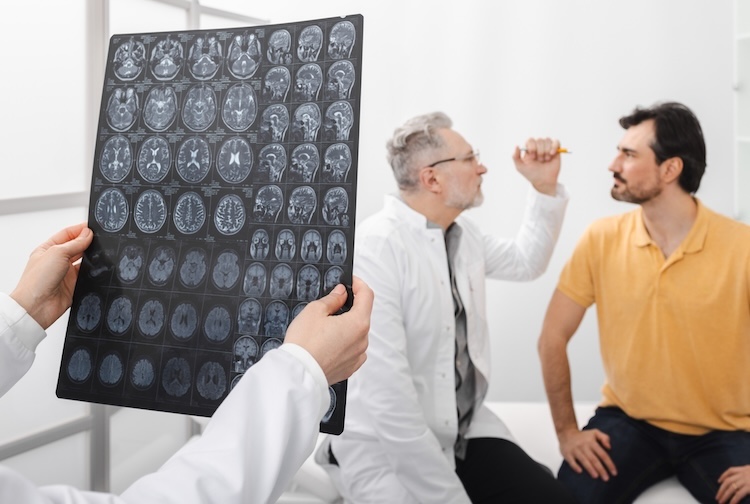
When it comes to clinical care, the landscape of Alzheimer’s disease has changed dramatically in the last five years. We’ve known for a long time how to spot signs of Alzheimer’s in the body, but it’s only recently that doctors have been able to use biomarkers, a measurable indicator of the condition, in everyday care. Today, imaging and fluid biomarkers can give us a better overall picture for diagnosis and progression.
At the same time, infusion therapies are being used and improved to fight the buildup of amyloid beta protein in the brain. Amyloid is one of the cardinal, pathological signs of Alzheimer’s disease. The infusions are able to remove them from the brain. In early symptomatic Alzheimer’s disease, it actually slows progression. These infusions are not cures; however, this is a very promising start.
Do you see lifestyle factors like sleep, diet and exercise playing a role in prevention or slowing progression?
The U.S. POINTER study, a trial that looked at accessible and sustainable lifestyle modifications to protect cognitive function, was released earlier this year and affirms that healthy lifestyle changes benefits brain health.
It doesn’t have to be hard or complex – just healthy. Some examples of healthy habits that can enhance brain health include regular walks, eating fruits and vegetables daily, and reading on a regular basis.
The sooner you can get started with these lifestyle adjustments, the better. Ideally, we want people in their midlife to reduce the risk of Alzheimer’s and related cognitive diseases by making some of these important changes.
What future treatments or research breakthroughs for Alzheimer’s disease are you most excited about?
While it was once believed that the only way to really diagnose diseases that cause progressive dementias was with an autopsy, that’s simply no longer true. And studies on the disease are moving the needle for faster diagnoses and treatment every year.
The next generation of amyloid targeting therapies is very exciting. We are seeing encouraging progress in trials that offer the hope of safer and more effective therapies in years to come.
Additionally, there are several clinical trials that involve medicines targeting facets of the underlying biology of Alzheimer’s disease. In the next 10 years, scientists anticipate having several different treatments that target those elements. Scientists are also getting much better at identifying and understanding the different brain changes that contribute to the disease.
What support does the VCU Health Alzheimer’s disease and cognitive disorders clinic provide for patients and families?
The first thing we will always aim to provide is a clear diagnosis. We want patients and families to be able to understand what the causes of their symptoms are and understand what the diagnosis means for their life, both now and in the future. We will be able to connect families with community support and will have social work support to help families navigate the challenges that arise. Some patients may return to their referring clinician with a diagnosis and a recommended care plan, while others remain within our clinic and receive ongoing supportive care.
What advice would you give to someone newly diagnosed with Alzheimer’s or related dementia, as well as family members and caregivers?
For patients, the prognosis and symptoms of this type of disease are dynamic. They can change depending on the stage of the illness. At the earliest stages, there may be minimal impact, but most of them are progressive. Understanding what that means and acting now to ensure that your preferences can be followed as your disease progresses is important.
For loved ones, it’s important that they give themselves time to grieve and process the diagnosis. There is no “right way” or “wrong way” to experience this illness. Take time to understand what medicine can and cannot do given your loved one’s particular diagnosis.