The many faces of liver disease
Why is the new Stravitz-Sanyal Institute for Liver Disease and Metabolic Health so important? Meet some of our patients.
April 19, 2022 Mya Santini, a patient at Children's Hospital of Richmond at VCU, received two liver transplants at VCU Health Hume-Lee Transplant Center— one when she was 4, the other at age 15. Mya suffered from autoimmune hepatitis when she got her transplants.
Mya Santini, a patient at Children's Hospital of Richmond at VCU, received two liver transplants at VCU Health Hume-Lee Transplant Center— one when she was 4, the other at age 15. Mya suffered from autoimmune hepatitis when she got her transplants.
By Esther Benenson
Liver disease. It's something few people talk about. But the causes of liver disease are many — not just alcohol. And no matter what the cause, we at VCU Health believe every life is special. That's why we're dedicated to providing the best care possible to all our liver patients.
And that's why we've established the new Stravitz-Sanyal Institute for Liver Disease and Metabolic Health. Through a $104 million gift from VCU Health liver specialist Dr. Todd Stravitz and his family's Barbara Brunckhorst Foundation, the Stravitz-Sanyal institute will transform health care as we know it.
And not just for liver patients. Liver disease is often a catalyst for heart disease, high blood pressure, diabetes and kidney disease — even Alzheimer's. So no matter which liver-related illness you or your loved one may have, the institute's focus on research, training and treatment will help.
Even before December 2021, when the institute was founded, VCU Health was known as a trailblazer in liver research and treatment. Whether patients entered through the hepatology department, our Hume-Lee Transplant Center or Massey Cancer Center, VCU Health teams collaborated to improve quality of life and save patient lives.
The Stravitz-Sanyal Institute for Liver Disease and Metabolic Health will undoubtedly accelerate the pace of innovation. It's dedicated to exploring the causes of liver disease and how to stop, prevent and even reverse it.
“It is urgent that we engage in more research to find better treatments,” said VCU Health liver specialist Dr. Arun Sanyal, who is leading the new institute. “Our institute will end up saving hundreds of thousands of lives in this country and perhaps millions around the world.”
Right now, the only cure for end-stage liver disease is transplantation. Across the United States, approximately 9,000 liver transplants take place each year. Many more could take place, but there aren't enough donors. Patients in need span all races, ethnicities and other demographics. Rich, poor, urban, rural, gay, straight — they could be your neighbors.
Here are the stories behind some of our patients:
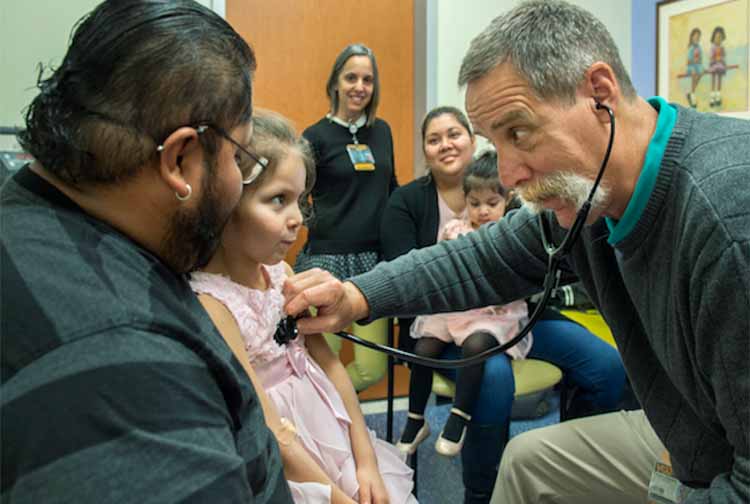
Astrid Cubas-Sanchez: Even children get liver transplants
Astrid Cubas-Sanchez was just 4 years old when she had her liver transplant.
Astrid was suffering from a rare genetic disorder, maple syrup urine disease, named for the sweet smell of the patient's urine. If left untreated, the disease can be deadly. Even with treatment, the metabolic condition can impose a variety of symptoms. For Astrid, it meant life with a gastrostomy tube (G-tube) to deliver nutrients directly to her stomach. She experienced a seizure and stroke, and her life was full of stringent dietary restrictions.
“I couldn't stand seeing my daughter the way she was suffering,” said her father, Jorge Cubas.
Hume-Lee Transplant Center coordinated with Children's Hospital of Richmond at VCU to perform the transplant, which took place in October 2018.
“I can't really believe it,” Jorge said at time. “She's doing wonderfully. When someone meets her and I tell them what she's been through, they can't believe it. They say it's unbelievable. … She has a new life.”
Adam McLean: Air force commander and “stress coach” extraordinaire
As an Air Force commander and human performance specialist, Adam McLean uses his Ph.D. in performance psychology to coach others — soldiers, airmen, businesspeople — to succeed in high-stress situations.
 But two years ago, as his cirrhosis worsened and he prepared for the end, Adam found himself needing a dose of his own medicine. His doctors in Orlando said there was nothing more they could do. So Adam, a 52-year-old Air Force veteran, had gone home to — as the doctor put it — “enjoy your family.”
But two years ago, as his cirrhosis worsened and he prepared for the end, Adam found himself needing a dose of his own medicine. His doctors in Orlando said there was nothing more they could do. So Adam, a 52-year-old Air Force veteran, had gone home to — as the doctor put it — “enjoy your family.”
But the air force commander wouldn't give up without one last fight. Through a twist in fate, one of his nurses suggested he contact the Veterans Health Administration. He did. And the rest is history.
In September 2020, Adam ended up at the Central Virginia VA Health Care System (CVHCS) in Richmond. CVHCS has a long-standing academic and medical partnership with VCU Health. Nine days after his arrival in Richmond, Adam received his liver transplant at VCU Medical Center.
“To be given that chance and new lease on life is absolutely humbling,” Adam said. “The people who are organ donors, and then the professionals who can make the transplant happen, are truly doing amazing work and are genuinely selfless.”
Throughout his transplant journey, Adam used every strategy in his stress management arsenal, from regulating his breathing and emotions to accepting things for what they are and bringing it all back to neutral.
Did his methods work?
“It's gotten me this far,” he said, with a laugh.

Steven Bennett: Performer, teacher
Music is Steven Bennett's passion. The talented guitarist enjoys playing classical, country, jazz and blues.
Steven shares his love of music by instructing students of all ages. He also plays gigs — from concert venues and weddings to local charity concerts raising funds to treat an assortment of health conditions.
“I've always done benefits, never thinking I'd be the one needing that care,” Steven said.
But when he did, he went to VCU Medical Center. The 32-year-old had pushed his liver to failure due to alcohol abuse. Steven desperately needed a liver transplant.
As part of an ongoing effort to provide holistic transplant care, VCU Health Hume-Lee Transplant Center offers a unique program to transplant patients like Steven who suffer from severe alcoholic hepatitis — a condition that often disqualifies patients at other centers.
“By working with addiction medicine specialists, alcohol counselors, social workers, hepatologists and surgeons, we're able to give some of these patients a second chance,” said Dr. David Bruno, surgical director of adult and pediatric liver transplantation at the VCU Health Hume-Lee Transplant Center.
With the support of his addiction medicine team, Steven got his transplant.
“It's a huge blessing,” Steven said. “[But] someone had to go through one of the worst possible things, losing a family member or a child, for me to live. And I put myself in this situation. … Before my liver failed, I wanted to get better. I just didn't know how.”

Karen Luper: Son donates liver segment to save mother's life
Karen Luper and her son, Brent Luper, had always been close. So when her liver gave out from decompensated cirrhosis in 2020, Brent selflessly gave her part of his own.
Karen had had liver disease for about 15 years. When she took a turn for the worse, she didn't have time to wait for a deceased organ donor. At the time, there were approximately 12,700 people on the national liver transplant waiting list. The year before, only 8,243 liver transplants had taken place using deceased donors, and nearly 1,200 patients had died waiting. Another 1,186 had become too sick to undergo surgery and were taken off the waiting list.
Despite a shared gene pool, the donation wasn't without complications. Karen and Brent had different blood types — something that usually ruled out a transplant. It wouldn't deter the team at Hume-Lee, though.
“We didn't have the luxury of waiting,” said Dr. David Bruno, surgical director of adult and pediatric liver transplantation at VCU Health Hume-Lee Transplant Center. “We were faced with a nearly impossible situation and had to overcome that in order to save Karen's life.”
Hume-Lee was one of the first transplant centers in the nation to overcome what's known as an ABO mismatch. It was a complex surgery, but Karen pulled through. She and her son are both doing well.
Sign Up for Transplant E-Newsletter




