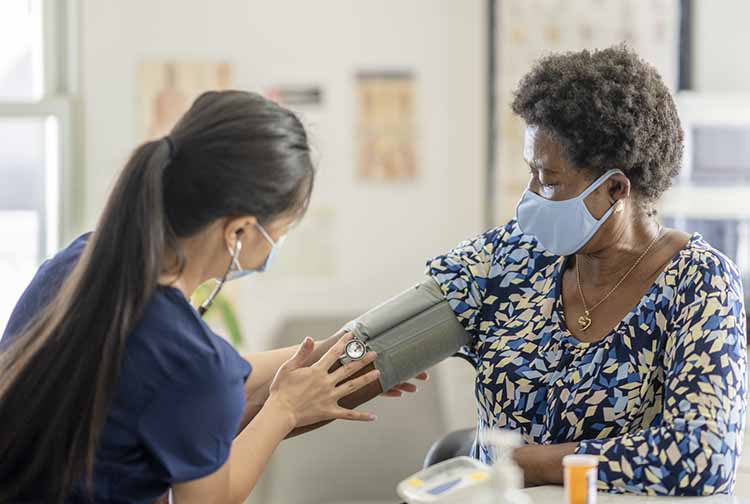

We combine clinical expertise, robust rehabilitation and emotional support to treat our COVID-19 patients.
COVID-19 hits the young, the old and the in-between. Be vigilant and follow standard safety practices. And don't delay care. When Corrine Townsend, right, came down with COVID-19, VCU Health took charge of her treatment. Corrine is now home with her husband and sons and is leading a full life.
Check for COVID-19 symptomsCurrent COVID-19 vaccine eligibility

For our patients:
- Local pharmacies and many local health districts now routinely offer vaccination appointments. Please visit vaccinate.virginia.gov or call (877) VAX-IN-VA or (877) 829-4682, Monday - Friday from 8 a.m. to 6 p.m., for a location near you.
- Existing VCU Health patients can call their primary care provider to schedule a vaccination or booster shot appointment.
- Pediatric patients see the CHoR blog for more information on COVID-19 and children.
- Immunocompromised patients may need to follow a different vaccine protocol. Please consult your doctor for more information.

For members of the community:
It is our mission to serve all Virginians. This includes a deep commitment to protecting our most vulnerable community members.
- To find other locations offering vaccinations, please use the following websites or text options:
- Please visit vaccinate.virginia.gov or call (877) VAX-IN-VA or (877) 829-4682, Monday - Friday from 8 a.m. to 6 p.m., for a location near you.
- The Richmond City Health District offers walk-up COVID-19 vaccination clinics. No appointment is necessary.
- Henrico County residents can call (804) 205-3501 Monday-Friday, 8 a.m. to 5 p.m. For help from the Centers for Disease Control and Prevention (CDC), you can text your zip code to GETVAX or 438829 (English) or to VACUNA or 822862 (Spanish).
COVID-19 News
Read the latest news, information and updates on COVID-19.

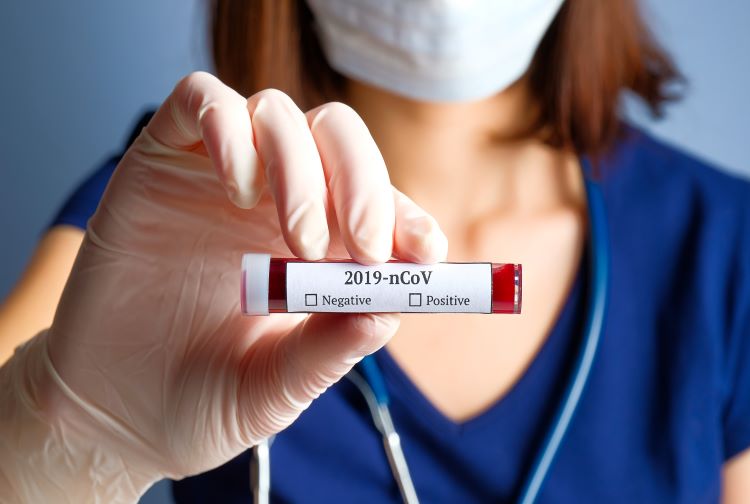



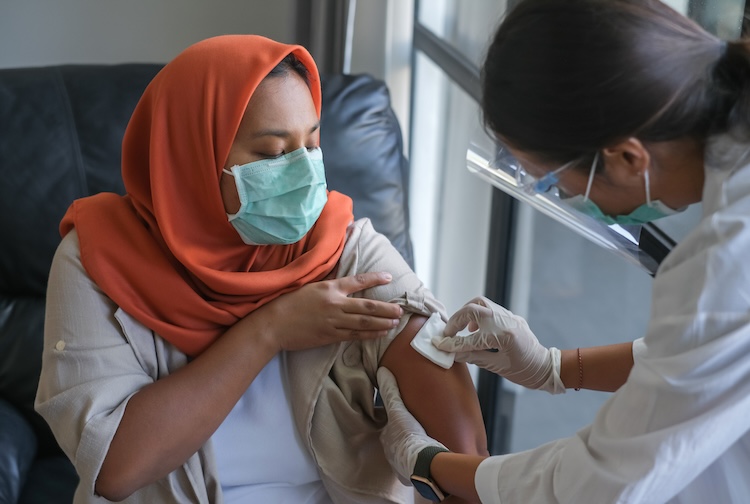






Urgent clinic virtual visits
Speak to a provider with our on-demand urgent clinic available to adults with no appointments necessary.
VCU Health MyChart TelehealthAppointments
Contact us to schedule an in-person or telehealth appointment from the comfort of your home.
Request an Appointment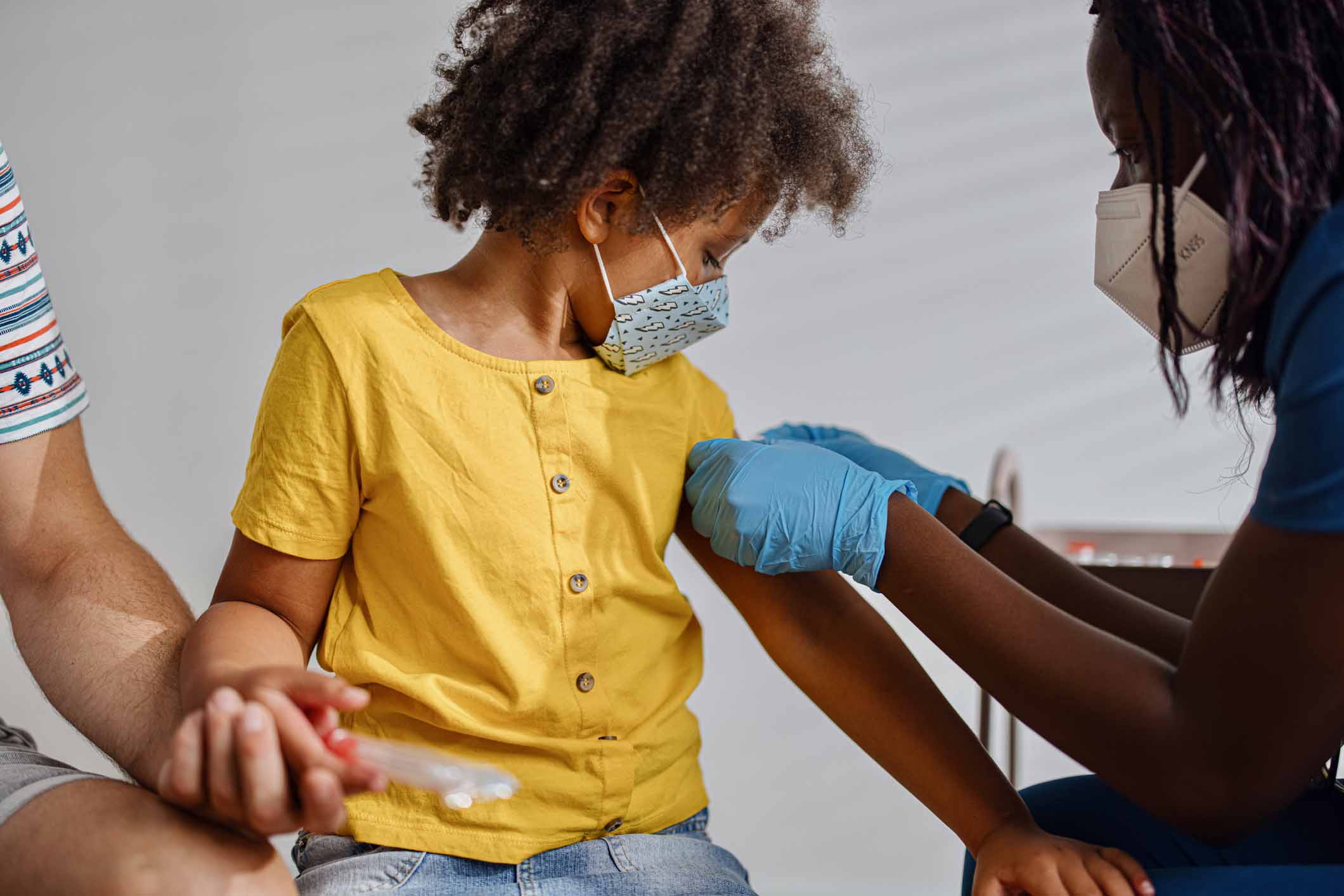
Pediatric vaccination
We are currently vaccinating children ages 5-17 their and caregivers. For more information, please visit:
Children's Hospital of Richmond at VCU (CHoR)COVID-19 Vaccine Frequently Asked Questions
Why should I get the vaccine?
COVID-19 isn’t the same as the flu. It’s extremely dangerous — to you and those you come in contact with. More than 50,000 people have died of COVID-19 in the United States.
If you develop severe symptoms from COVID-19 and survive, your recovery typically isn’t easy. You may require lengthy, difficult rehabilitation.
Now that vaccines are available, don’t take chances. Get the vaccine — to protect yourself, your family and the surrounding community.
Are the COVID-19 vaccines safe?
Yes. The COVID-19 vaccines are safe. The Centers for Disease Control and Prevention has approved all three vaccines available in the United States — Pfizer, Moderna and Johnson & Johnson (J&J).
To be approved, vaccines must go through a careful trial process with several phases to address safety and effectiveness. The COVID-19 vaccine trials did just that, and they included an extremely large number of participants. There were at least 30,000 people each in the Pfizer and Moderna trials, and 43,000 people in the Johnson & Johnson trials.
The COVID-19 vaccines were produced so rapidly not because they were rushed by cutting corners but because scientists had significant prior experience working with other coronaviruses, such as SARS (severe acute respiratory syndrome) and MERS (Middle East respiratory syndrome). Research on a COVID-19 vaccine did not start from scratch.
In addition, the U.S. government made vaccine development a priority once the COVID-19 coronavirus took off in the United States. We also have a huge amount of real-world experience with the vaccines now, and the vaccines have proven to be incredibly safe.
How effective are the vaccines?
The COVID-19 vaccines are highly effective at preventing symptoms, hospitalizations and death. However, the strength of the vaccines does decline over time. The U.S. Department of Health and Human Services now recommends a booster shot for everyone who received the full two doses of the Pfizer or Moderna vaccine or the one-dose Johnson & Johnson vaccine.
Does it matter which vaccine I get?
No. All three vaccines (Pfizer, Moderna and Johnson & Johnson) are excellent at protecting you against COVID-19. Take whichever vaccine is offered to you.
Are there side effects?
As with most vaccines, you may experience mild to moderate side effects. These can include fatigue, mild fever, headache, muscle aches and pain in your arm at the injection site. These side effects may last a couple days but are completely normal.
Are there possible allergic reactions?
As with any medication, some people may experience an allergic reaction to the COVID-19 vaccine. This risk is extremely small. To be on the safe side, health care workers may ask you to remain for a short period after your vaccination so they can monitor you for an allergic reaction and take action should one occur.
If you do suffer an allergic reaction, contact your doctor, as you may want to skip the second dose of the vaccine. An allergic reaction is considered severe if you require epinephrine or an EpiPen for treatment or you need to go to the hospital.
Can I get COVID-19 from the vaccine?
No. You cannot get COVID-19 from any of the vaccines. None of the vaccines contain the live coronavirus nor do they contain a weakened or dead version of the coronavirus. The vaccines have no coronavirus to pass on to you.
What if I'm pregnant?
The vaccine is safe and highly recommended for the protection of you and your unborn child. Please see COVID-19 vaccine and pregnancy: Should I get the vaccine? and COVID-19 and pregnancy: Virus can be deadly.
Do I need a booster shot?
Once I get the vaccine, can I stop wearing my mask?
Not entirely. None of the vaccines are 100% effective. Although vaccination is associated with a marked reduction in severe infection, we now know that breakthrough infections can occur. When these happen in vaccinated people, they tend to be mild — but infected people can still spread the virus to others. People who are unvaccinated, those who are immunocompromised and the elderly — even if vaccinated — are especially at risk of catching the virus from people with breakthrough infections.
It usually takes two weeks after you complete your vaccine series to acquire immunity to the virus that causes COVID-19. You could get infected during this time, endangering your health. You might also still be able to spread the disease, both during this 2-week window as well as after you develop full immunity, endangering others.
With COVID-19 activity still strong, wearing a face mask is critical to preventing the spread of disease.
This is particularly important in indoor public spaces, but also in outdoor spaces where you cannot maintain 6-foot distance from others. You should mask regardless of whether or not you are vaccinated. To the extent possible, you should also practice social distancing, avoid crowds and wash your hands often.
If I've had COVID-19, do I still need to get vaccinated?
We recommend you get the vaccine. Reinfection is possible. Some experts recommend waiting three months from when you developed COVID-19. This is because you probably have some degree of natural immunity. Importantly, it is not clear how long natural immunity will last. If you are in this three-month window, you should discuss the best time to get the vaccine with your doctor. If you've had symptoms of COVID-19 but were never diagnosed, don't assume you had the disease and are immune. Get the vaccine.
Will the vaccines protect me from omicron variant? What about new variants that come along in the future?
All COVID-19 vaccines available in the United States protect against the dominant variants in the U.S., including omicron. If you do get infected, your symptoms will likely be mild. By getting vaccinated, you reduce your risk of severe COVID-19, hospitalization and death. You also help prevent viral spread and thereby limit the emergence of new variants.
How do I get the vaccine?
If you are a patient at VCU Health, you may get the vaccine here. Please call us at (804) 628-0223 to schedule your vaccination. Calls are taken Wednesday-Friday, 8 a.m. to 5 p.m. Appointments are required. Walk-ins are not accepted.
Vaccines are also widely available in the community. Visit vaccinate.virginia.gov to find places near you that offer the vaccine.
Where can I find more information?
Please continue to check our COVID-19 website, as we are constantly adding new information. Also sign up for our monthly e-newsletter.
Are you a current or prior bone marrow transplant or CARt patient?
Specific guidelines on vaccination timing, vaccine type and follow up after COVID-19 vaccination exist for patients after CARt, autologous or allogeneic transplants. Call the cellular immunotherapies and transplant program (CIT) COVID vaccination line at (804) 628-7290 to get clearance and vaccine access to ensure the best benefit and safety for your specific situation.
For information on pediatric vaccinations.
Please visit Children’s Hospital of Richmond at VCU.
For information for cancer patients.
Please visit VCU Massey Cancer Center.
For information on COVID-19 and other medical conditions.
Please visit Patients with specific medical conditions..

A message from your Family Medicine team
Your Family Medicine team is committed to providing you the safest possible care.
Family medicine message
Vaccine Champions
Together, we can help support the health and wellbeing of our community.
Learn about our Vaccine Champions program
Sign Up for COVID-19 and Vaccine Updates
Subscribe to receive our emails, alerts and newsletter updates.
Subscribe for updates



