On a rainy morning 26 years ago, I was instantly transformed from an athletic young guy into an aching old man.
I was exercising at home, running in place while curling hand weights, when I was stricken with excruciating low-back pain.
I was 42. I liked to run, backpack, paddle in white water and play softball. All of that ended immediately.
Now I’m 68, and in those intervening years, I have tried everything from surgery to acupuncture to having an electric pain blocker implanted in my back. (The rectangular bulge from that device is a bad look at the pool.)
Nothing worked.
I have encountered people who attributed my plight to godlessness, asked about suicide, told me everything happens for a reason and suggested all sorts of sure-fire cures — as well as people who are caring and kind.
People are also reading…
So it was with great hope that I recently began my final quest, most likely, to end the pain. I went into VCU Medical Center for an unusual three- to five-day trial, or test, to see if pumping morphine directly into my back would help.
The plan was for my doctor to surgically implant a catheter, or tube, into my lower back — right through a tough membrane along the spine and into the spinal fluid. The tube — a tiny thing resembling a fishing line — would be attached to a little machine that pumped out the morphine.
By going into my back, and not more directly into my blood through pills, the morphine was supposed to be more effective, while not getting me high or addicting me.
If this test was successful — if the morphine beat back the pain — my doctor could later implant a morphine pump into my lower back. After all these years, I would be out of pain, or close to it.
I had endured nothing but disappointment in the past, but this looked promising. We know morphine kills pain. Morphine pumps have worked with cancer patients.
I was excited.
***
My doctor says he has never seen pain like mine. It comes and goes like clockwork.
If I sit or get on my feet — standing or walking — the pain starts at a low level but rapidly grows worse and worse. That pain ratchets up — minute by minute, almost — toward infinity, it seems.
Over the course of an hour or two, the sensation goes from uncomfortable, to painful, to unbearable, and the pain keeps climbing until I find a place to lie flat or recline.
Once I get flat, or close to it — on a couch at a relative’s recent funeral, for example, or in the leaves along the Appalachian Trail — the pain oozes out like air from a punctured tire. The feeling is euphoric.
I can tough it out through a restaurant dinner. I can tough it out through a movie. But I haven’t done dinner and a movie in 26 years.
I was a reporter for years at the Richmond Times-Dispatch. The paper was nice enough to get me a plush reclining chair — the “Captain Kirk chair,” newsroom friends called it. I would come back from covering the state Waste Management Board or whatever, then lie back and let the pain hiss out while I wrote my story.
If I am horizontal long enough — it takes hours, sometimes — my pain will disappear. My heart goes out to people with pain they can’t escape.
Experts say 8% of American adults suffer continuing back pain, some worse than others. Many more people endure pain from other causes. We are a large club, open to anyone.
People always ask what causes my pain. Among other problems, I have degenerative disc disease, which means those tough little pads between my vertebrae are wearing out. But lots of people have this ailment and suffer little pain.
In many ways, my pain is a mystery.
***
My long battle against pain has kept me close to VCU Medical Center. I had surgery there in 1994. No help.
I got through my working years mainly with meds — primarily the prescription painkiller tramadol but also ibuprofen and Tylenol — to ease the pain.
I retired from the RTD about four years ago, and suddenly I had time to explore new options. My doctor at the time, neurosurgeon Bruce Mathern, suggested I enter a VCU Health pain clinic.
That led to my current doctor, VCU pain specialist Andrew Chapman, a friendly, brown-haired man and former Army flight surgeon. Starting about three years ago, Chapman led me methodically and conservatively through measures including physical therapy, shots and the acupuncture.
Another VCU doctor did the acupuncture, inserting short, flexible needles into my back and sides and leaving me to relax face-down on a table for 20 minutes or so with soothing music and low light. I got cold, but not out of pain.
When those things didn’t work, Chapman suggested an electronic pain blocker, called a neurostimulator — a little rechargeable power pack that would send electric pulses into two wires inserted along my spine. The pulses were designed to interrupt the pain signals.
First, Chapman put me through a test, with the device strapped to my back for several days. The arrangement seemed to reduce my pain — finally, something worked — so Chapman implanted the device, slightly smaller than a cigarette pack, in my lower left back.
Looking back on it, the relief I felt during the test was probably a placebo effect. The neurostimulator was a flop. Today, that hard little device remains just under my skin, doing nothing.
Beyond heavily invasive surgery that could make me worse, I was down to one option — the morphine pump. Chapman wanted to test it on me — with the pump outside my skin — in the hospital for three to five days. In these days of in-and-out medicine, that long a stay would be unusual, but Chapman said it would yield a better picture than a quick look
It was time for the test.
***
Chapman put the tube in my back during an operation shortly after dawn on a Monday in February. Afterward, he wanted me to walk a lot around the hospital. Walking normally caused pain, remember, but if the morphine worked, I should feel pretty good on my travels.
During the entire multiday test, I would be tethered by the tube to a rolling stand that carried the morphine pump.
This might sound weird, but I thought the experience would be fun. I would be walking around the hospital, chatting with nurses and patients and racially profiling for Latinos with whom I could practice my Spanish. The only downside could be finding that the morphine didn’t help.
On my first walk after surgery, back when walking around a hospital wasn’t the worst idea in the world, I felt so good that my wife, Kathy, took a photo of me “pole dancing” with the morphine stand.
My experience in the hospital was days before the coronavirus began dominating our lives. Nothing here is meant to disparage that horror, which is creating a growing list of victims and heroes.
***
Well-meaning people say the darnedest things.
“There are no coincidences.”
“Everything happens for a reason.”
“Time heals all things.”
If you cross the street and get hit by a car, did that happen for a reason? Absolutely, if you weren’t paying attention or the driver was texting. But those reasons aren’t sufficiently otherworldly for people who say these things.
One person suggested God was punishing me for not sufficiently honoring him. Who would worship such a god?
Then there are those who hold the secret to curing your pain. I’ve heard yoga, Feldenkrais exercise, swimming the backstroke (really), acupuncture (a big flop) and more recently CBD oil and weed. The weed sounded the most intriguing.
I could see myself at 80, down to seeds and stems.
***
Shortly after my happy pole dance, it all changed.
I got god-awful, never-forget-in-my-life nausea, a reaction to the morphine. I threw up over the next two days like I’d been to 10 keg parties each day. I was the kid who vomited like a fire hose in the movie “Stand By Me.” I recognized all my hospital food, which was good — the food, that is.
Try making an emergency dash to the toilet while dragging a morphine stand.
The drugs I was fed — the morphine stream and maybe some of the anesthetics from surgery — had the additional benefit of making me unable to urinate, which is a whole ’nother type of discomfort. Once, a male nurse helped by a female nurse inserted a urine-draining catheter — something you strangely want and don’t want at the same time.
On top of all that, I got a searing headache, apparently from dehydration. And I had the chills.
It was hard to enjoy “Gunsmoke.”
***
Pain makes you have thoughts you’re not proud of. I once saw a news story about a wounded warrior who could ski on one leg and thought: Shoot, I’d give up a leg to get back my back. Would I give up an arm? No. An eye? Maybe.
Then I’d see a story about someone who lost a leg or arm but still felt pain where it used to be and think: That person really got screwed.
Then there’s the suicide thing. Anyone who has suffered long-term pain and not thought of ending it forever is stronger than me.
Back when my pain was new — when my happy life turned to misery — suicide crept into my thoughts a lot. Those thoughts decreased over time but never went away. I’ve gone so far as to think: “If I kill myself, will my wife get my life insurance?” Then I’d think, “If I drown in the James River, and it looks like an accident, then will she get the money?”
What’s crazy is that my life insurance policy is worth only about $1,000 or so. The payoff wouldn’t be worth the effort.
Sometimes I’ve thought of buying a gun. But you know what? A depressed friend shot himself in the head with a handgun and survived. He’s disabled now, but he seems happier. Everything happens for a reason.
To be clear, my suicidal thoughts have been more like strange mind games than real plans.
As part of my treatment, the VCU pain clinic folks sent me to a psychologist not long ago. I took some tests, chatted with the psychologist and told her about my occasional dark thoughts. She said I was normal and needn’t return.
I think she was right.
***
In my room, the morphine kept coming, and so did the nausea.
After I had thrown up for those two days, Chapman switched my feed to Dilaudid, a less-serious but still heavy-duty opioid. The vomiting stopped, but the nausea continued. Then the dosage was reduced to a tiny concentration.
I was still sick.
Late on the fourth day, Chapman pulled the plug.
The test had failed.
Chapman said he had never seen anyone so sensitive to opioids. Once again, I was special. What’s more, the drugs had alleviated little of the pain.
The week had been a nightmare, but for most pain sufferers I suspect my experience rings truer than all those “medical miracle” stories you see.
Time and doctors don’t heal all things.
***
Sometimes, even when life is dismal, you can’t help but laugh.
When I couldn’t urinate, the nurses scanned my bladder several times to see how full it was. Inserting a catheter to drain urine, I learned, is no small thing because it can cause infection. You have to be really, really full to get the relief of the catheter, no matter how miserable you feel.
The nurses scanned me with a device that resembled a hand-held mic. They poked this cold thing into various parts of my lower belly, which made me want to go even more.
These scans produced blob-like screen images that looked to me like cartoon pools of urine. What really cracked me up was that these computerized blobs were yellow.
Maybe it was the drugs.
Each scan produced a number — for milliliters of urine in the bladder — and I couldn’t get the catheter until I “hit 300.”
I wasn’t very good at first, hitting below 250, but over the course of a long afternoon my performance improved. When I finally hit 300, I felt like I had won the batting title.
My favorite question from a nurse: “Do you have trouble passing gas?” Kathy knows the answer to that.
Kathy stayed with me the full 4½ days, sleeping in a not-great chair. Our private, 11th-floor room had a big window overlooking an office building, and we spied on people like the characters in “Rear Window.” We didn’t see any murders, but one time a woman who had been desk-bound nearly all day got up just before 5 p.m. and did some sort of disco dance.
It was better than my pole dance.
***
I was discharged on Friday afternoon, groggy but only mildly nauseous. As a parting gift, I had an even worse headache, probably from leaking spinal fluid. That headache persisted for more than a week.
Before leaving the hospital, I consulted in my room with two doctors, one a woman and the other a man. The conversation included:
Her: “When you get home, you can do anything you want.”
Me: “Can I play the piano?”
Her: “Sure.”
Me: “That’s great. I never could play the piano before.”
Him: “I can’t believe you fell for that one!”
He said it twice.
***
My dream of relief had gone poof.
On the other hand, there was a woman in a nearby room who moaned all night with pain. No matter how bad you think you’ve got it, there is always someone else who has it worse.
Medically, the back-pain test was a nauseating failure, but there were benefits. I have a deeper love for my wife (which I thought was impossible). I am full of appreciation for those caring VCU nurses and doctors, especially Chapman. I relearned how great my friends are.
What’s next? Perhaps some adjustment of my painkillers. Walks among blooming flowers and singing birds, if the coronavirus allows.
And you know what? Being homebound because of the virus, I’m not sitting in restaurants with friends and doing all those things that kill my back. I feel pretty good.
Everything happens for a reason.
Rex Springston lives in Richmond’s Fan District. He searches for coffee shops with couches he can flatten into. You can contact him at crexs@aol.com.

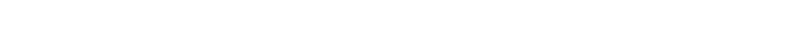












![A1 Minute! April 19, 2024: Week in Review[A1]](https://bloximages.newyork1.vip.townnews.com/richmond.com/content/tncms/assets/v3/editorial/2/b1/2b170387-5138-5d02-9d6e-60bcc76e33ad/6622c307d9775.image.jpg?resize=150%2C84)
![A1 Minute! March April 19, 2024: Warm, dry conditions for 10K race; Virginia Sports Hall of Fame; Top 5 this weekend[A1]](https://bloximages.newyork1.vip.townnews.com/richmond.com/content/tncms/assets/v3/editorial/7/d0/7d03a017-d968-514e-9456-1877f20cedf6/66227580dcf1c.image.jpg?resize=150%2C84)
